Eye Surgery
Cataract Surgery
Intraocular Lens (IOL) Implant Surgery
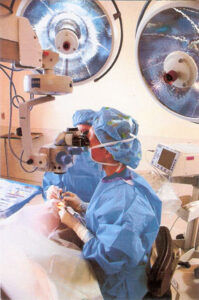 Most Americans between the ages of 65 and 75 have some degree of cataracts. It is completely up to you when the cataract is bad enough to want to have it removed. Some individuals only have minor cataracts and choose to wait till they worsen before the procedure. Others choose to get their full vision back right away.
Most Americans between the ages of 65 and 75 have some degree of cataracts. It is completely up to you when the cataract is bad enough to want to have it removed. Some individuals only have minor cataracts and choose to wait till they worsen before the procedure. Others choose to get their full vision back right away.
Cataract surgery is one of the most effective treatments for this condition. Over 95% of patients treated have better vision after removal of the cataract. The procedure involves a microsurgery under local anesthesia.
With cataract surgery, the cloudy lens inside your eye is removed and replaced with an artificial lens called an Intraocular Lens (IOL). It is an out-patient procedure with the whole process encompassing only a couple of hours.
There are varying types of IOL options available depending on your current vision deficiency. Your doctor will talk with you about which option might work best with your lifestyle.
Posterior Capsule Opacification (PCO)
A common experience from post-cataract surgery is the development of a secondary cataract. This complication is known as Posterior Capsule Opacification (PCO). The cause is the back of the lens capsule containing the IOL implant is now becoming cloudy and impairing vision.
This problem is also treatable with a painless and quick outpatient procedure called a YAG Laser Capsulotomy. The process consist of applying a laser cut making a clear path for light to pass through the clouded capsule.
Types of Intraocular Lens Implants
There are various options for the type of lens you have implanted. These may include a monofocal lens which allows you to see well at a particular focal point, such as distance (but still need to wear reading glasses for up close) or near (but still need to wear glasses for distance).
Multifocal Lens Implant
Implementing a multifocal lens provides both near and far vision to minimize dependence on glasses. 93% of patients with the ReSTOR multifocal lens implants never use glasses again to see far and 81% to see near.
Toric Lens (Astigmatism) Implant
A toric lens is ideal for those that also require correction of astigmatisms.
Glaucoma Surgery
Trabeculectomy is a microsurgical procedure that creates a small hole into the eye under a flap in the sclera to provide a new drainage pathway for fluid to exit the eye. Mitomycin is an anti- scarring medication used at the operation site to prevent the flap from scarring closed. Fluid from under this “trap door” flap then collects under the conjunctival tissue covering the eye. This bubble of fluid is called a “bleb” and is located at the top part of the eye under the upper lid. The fluid is then reabsorbed by surrounding blood vessels.
The Ex-press ® Mini Glaucoma Shunt surgery is performed similar to the trabeculectomy discussed above. The main difference is that it involves inserting a tiny metallic shunt in the hole between the inner and outer walls of the eye to create a new drain which bypasses the eye's damaged drainage system, allowing excess fluid to exit the eye. This fluid then forms a bleb and gets reabsorbed by the body.
Glaucoma Tube Shunt surgery involves carefully inserting a small tube into the front chamber of the eye, just in front of the iris. Fluid from inside the eye can then drain through this tube out of the eye to a reservoir which is formed by a silicone plate at the back of the implant which is affixed to the sclera. The fluid collects here and is then reabsorbed by surrounding blood vessels.
Corneal Transplants
Corneal Transplant candidates experience distorted vision from damage to the corneal lens. The cornea is the clear layer on the front of your eye that helps focus light. The procedure is known as a keratoplasty and there are varying degrees of performing this surgery. This form of eye surgery is an out-patient procedure only taking a few hours of time to perform. Recovery times vary depending on the type of transplant.
A full thickness corneal transplant, or Penetrating Keratoplasty (PK), involves replacing an entire cornea due to severe damage due to bulging or scarring from previous injury.
A partial thickness corneal transplant, or Deep Anterior Lamellar Keratoplasty (DALK), is where only the damaged layers of the cornea are removed. People with keratoconus or a corneal scar that hasn't affected the inner layers are good candidates for this form of surgery.
Endothelial Keratoplasty affects half of those needing a cornea transplant where there is a problem with the endothelium, or innermost layer of the cornea. This surgery is also ideal in helping those with Fuch's Dystrophy.
